Leg pain, aching, and cramping are often signs of underlying vein disease, a condition that affects blood flow in the legs. Poor circulation, varicose veins, and blood clots can disrupt the normal movement of blood back to the heart, leading to discomfort and potential complications if left untreated. These symptoms may worsen with prolonged standing or sitting and often improve with elevation of the legs.
A thorough evaluation is critical to understanding the root cause of your symptoms. Our diagnostic process includes:
We use cutting-edge, minimally invasive procedures to address vein-related issues effectively, helping you achieve symptom relief and improved circulation.
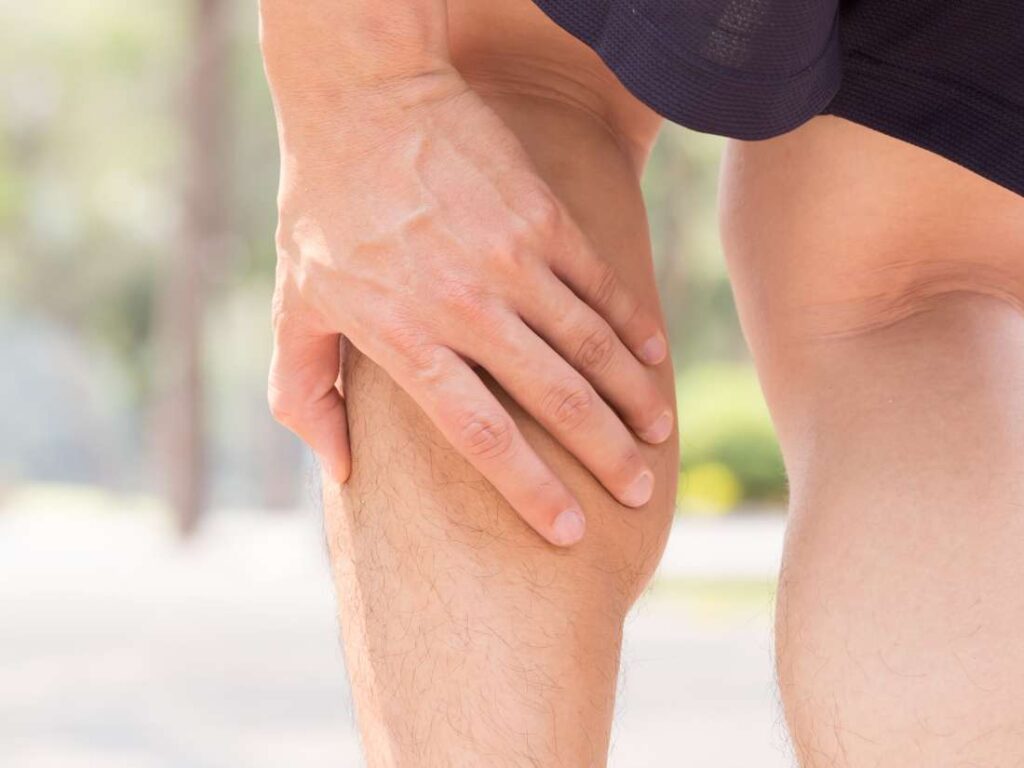
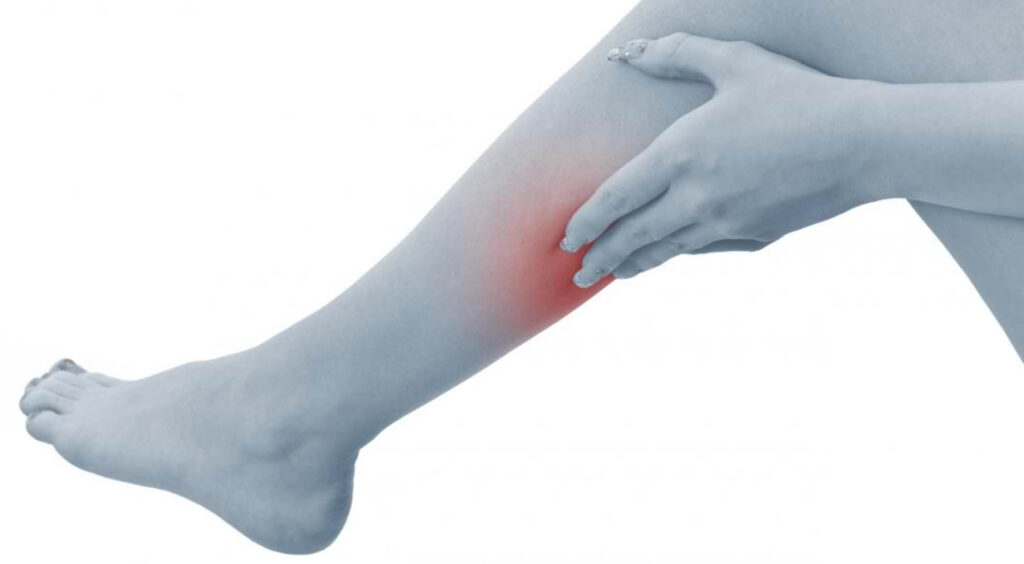
A comprehensive diagnostic process helps us determine the root cause of your skin changes and discoloration:
Our minimally invasive procedures address the underlying causes of skin changes while promoting healing and restoring a more natural appearance:
A comprehensive evaluation helps us identify the root cause of your swelling and create an effective treatment plan.
Our cutting-edge treatments target the underlying causes of swelling, providing relief and promoting long-term leg health:
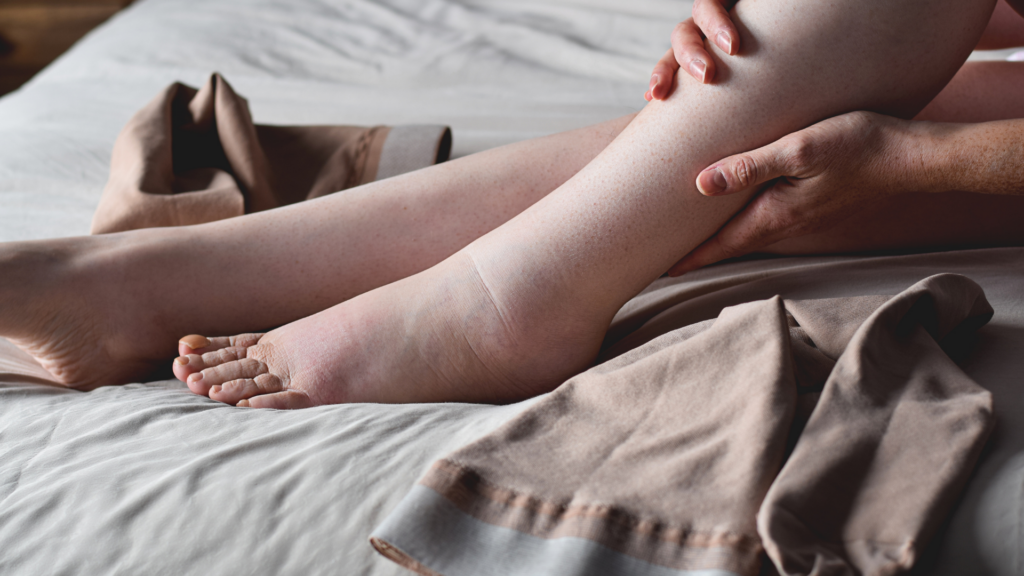
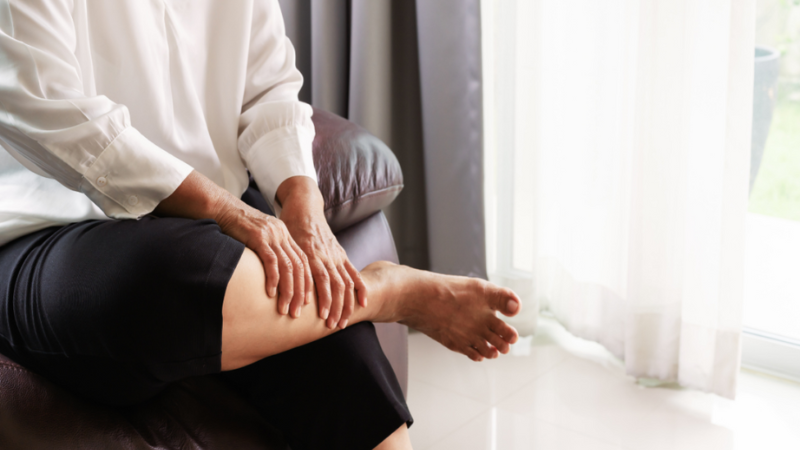
Our thorough diagnostic process ensures we identify the root cause of your symptoms and recommend the best course of action:
We offer state-of-the-art, minimally invasive procedures designed to improve circulation, alleviate symptoms, and enhance your quality of life:
Our diagnostic approach focuses on identifying the underlying cause of the wound to ensure effective treatment and faster healing:
We offer state-of-the-art, minimally invasive treatments that address the underlying vein disease while promoting faster healing of ulcers and sores:
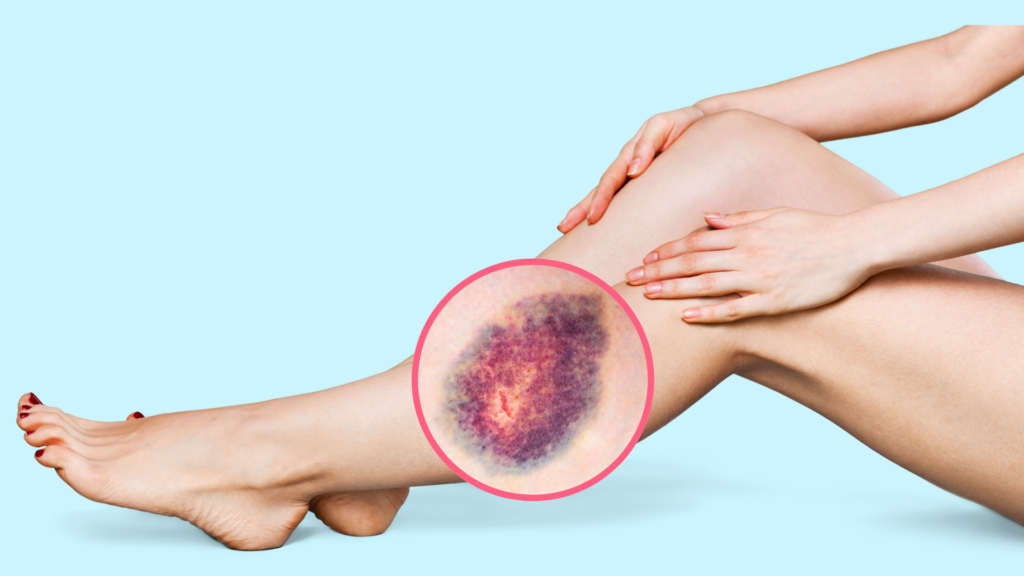

Restless legs syndrome is characterized by an uncontrollable urge to move the legs, often accompanied by uncomfortable sensations like tingling, itching, or aching. This condition is frequently caused by poor circulation due to vein disease. While medications may alleviate symptoms temporarily, they do not address the underlying circulation issues. Restless legs can be a sign of venous insufficiency, where blood flow is restricted, causing discomfort and interfering with sleep and daily activities.
Our diagnostic approach focuses on identifying the underlying circulatory issues contributing to restless legs, allowing us to recommend the most effective treatment plan:
We offer cutting-edge, minimally invasive treatments designed to improve circulation, reduce discomfort, and eliminate the root cause of restless legs:
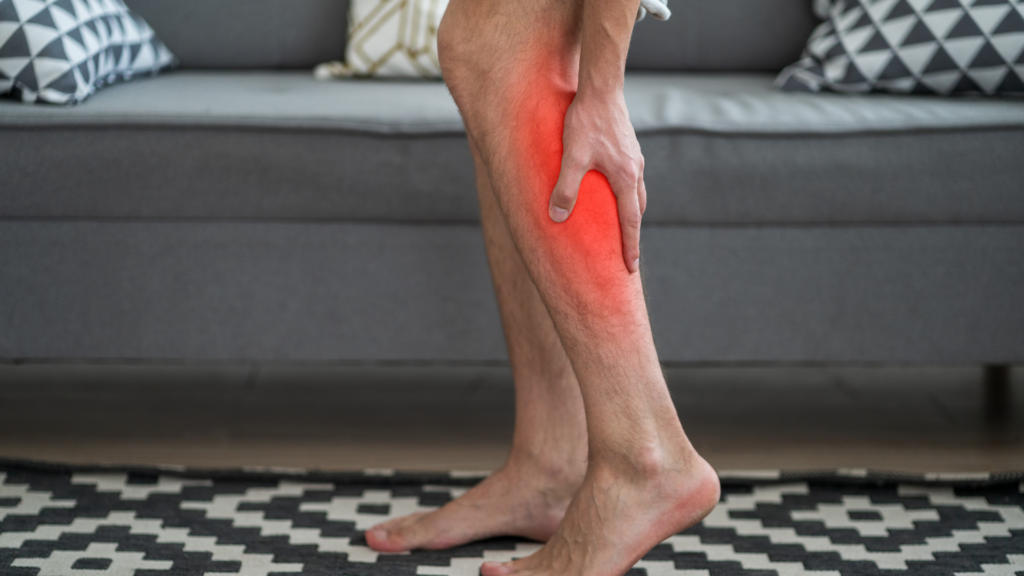
Tingling, burning, or itching sensations in the legs are often linked to poor circulation caused by vein disease. This discomfort occurs when blood flow is restricted, preventing nutrients and oxygen from reaching the skin and tissues. The sensation can range from mild to severe and may worsen after prolonged periods of sitting or standing. Tingling or burning in the leg is a common symptom of venous insufficiency, where the veins cannot efficiently return blood to the heart.
To effectively address tingling or burning in the leg, we focus on determining the underlying venous issue causing the discomfort:
Our minimally invasive treatments are designed to address the underlying vein issues, restore healthy blood flow, and relieve tingling or burning sensations in the legs:
Endovenous Laser Therapy (EVLT)
Closes damaged veins, improving circulation and reducing skin irritation.
Compounded Sclerotherapy
Targets smaller veins with injections to improve circulation and relieve discomfort.
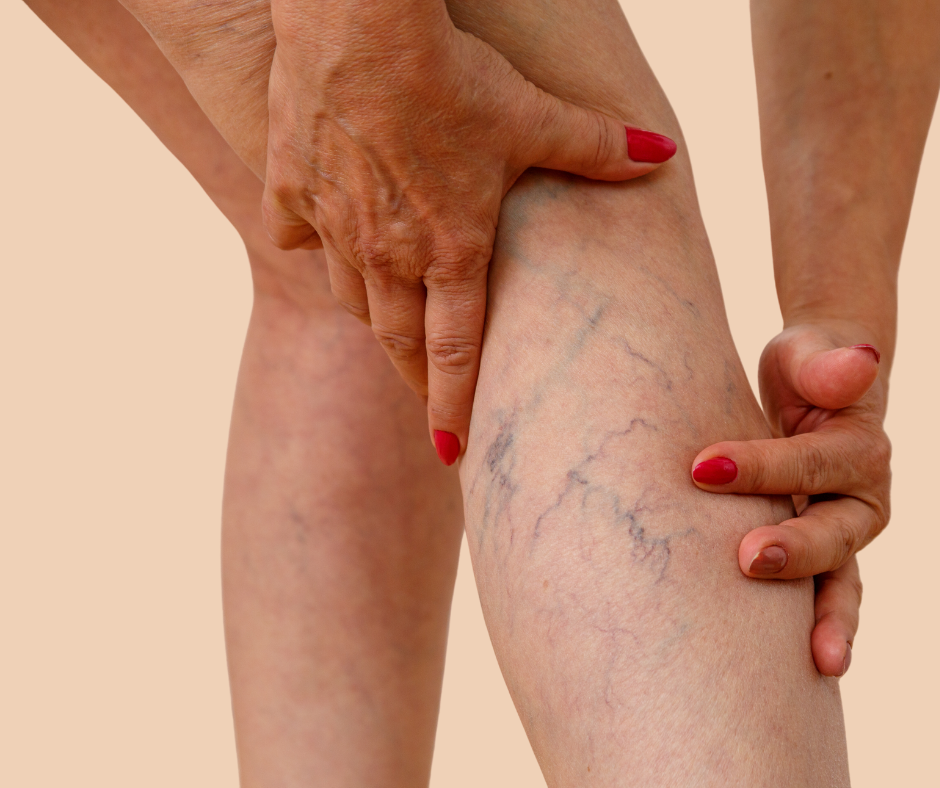
Varicose veins are enlarged, twisted veins that often appear bulging and blue or purple, typically in the legs. Spider veins, smaller and closer to the skin’s surface, may look like fine red or blue lines in a web-like pattern. Both types of veins are often caused by high pressure in the leg veins, which weakens the vein walls and causes them to stretch and become visible. While spider veins are usually a cosmetic concern, varicose veins can lead to pain, swelling, and more serious health issues if left untreated.
Our diagnostic process focuses on identifying the underlying causes of varicose and spider veins, allowing for the most effective treatment:
We offer minimally invasive treatments to eliminate varicose and spider veins while improving circulation:
Copyright © 2025 Trident Vein Center LLC, All Rights Reserved | Privacy Policy